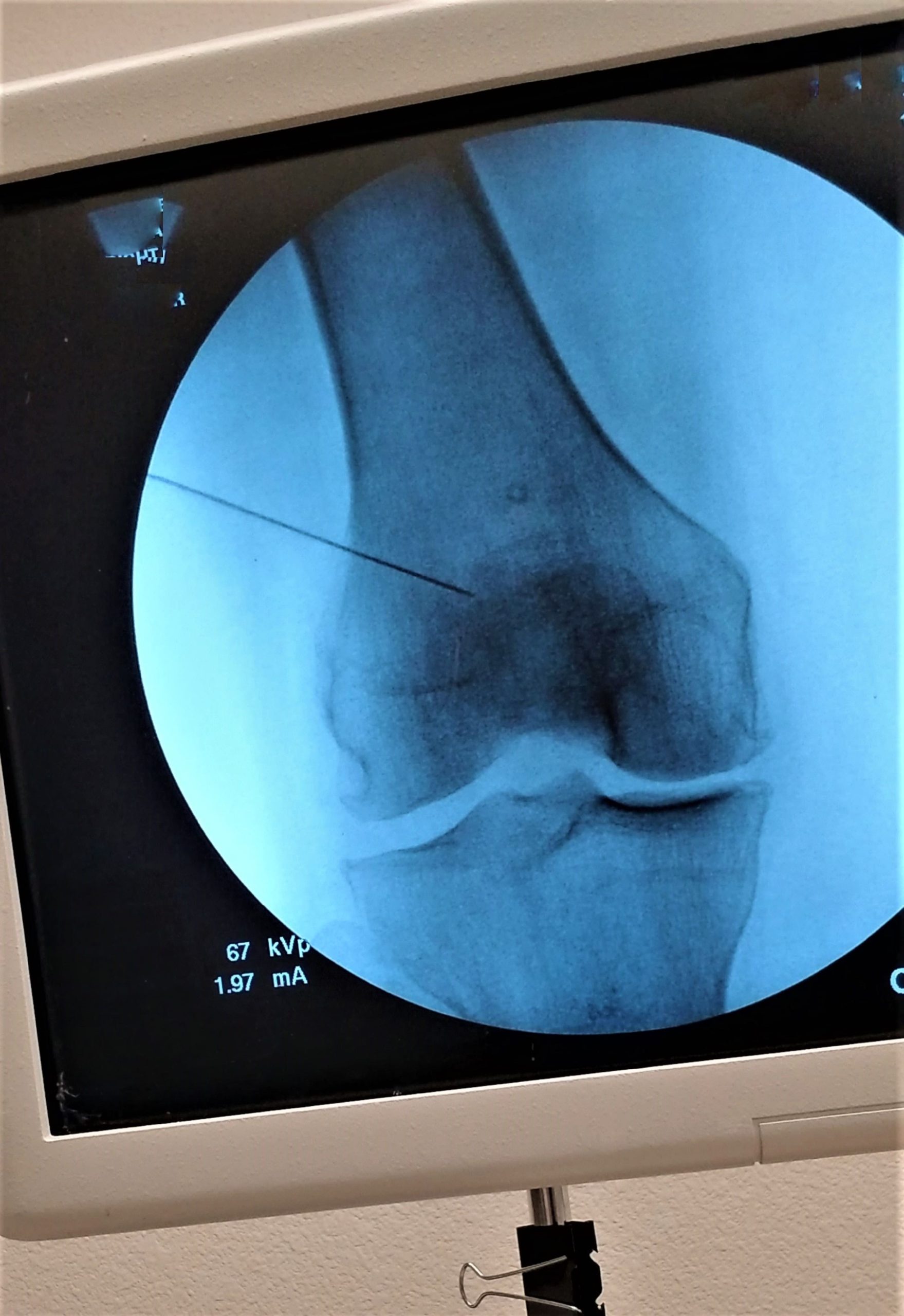
An osteochondral defect is a joint injury involving both the smooth articular cartilage and the underlying subchondral bone. Unlike isolated cartilage damage, OCD affects the bone’s structural integrity, often causing fragments to detach and form “loose bodies” within the joint.
The knee is particularly vulnerable to these defects—most commonly on the medial femoral condyle and the kneecap—due to the high mechanical forces it endures. This dual-layer damage creates a rough joint surface, leading to pain and potential long-term joint degeneration.
Patients with osteochondral defects typically experience:
- Deep knee pain
- Swelling
- Catching or locking sensations (the knee feeling stuck or giving way suddenly)
- Difficulty with weight-bearing activities (such as walking, climbing stairs, or standing for long periods)
Left untreated, these defects can progress to more widespread cartilage degeneration and early-onset osteoarthritis. Treatment aims to restore the smooth joint surface, promote healing of the underlying bone, and help prevent long-term joint deterioration.